Hematoma is the effusion of the blood from the vessels, due to any injury or puncture mainly during the administration of the Local Anesthesia. Check the section “Hematoma” for the causes, problems and ways to prevent the Hematoma formation. Below are the ways how one can manage the Hematoma if it occurs after the Local Anesthesia is administered. The two ways of management of Hematoma are:
a) Immediate Management of Hematoma due to Local Anesthesia
b) Subsequent Management of Hematoma due to Local Anesthesia
It depends a lot on the timing after the Local Anesthesia, when the Hematoma is formed and when you detect it. If at all the hematoma formation is detected immediately after the LA is administered, one can apply finger pressure on particular areas based on the LA given, but on the later stages there are different precautions and steps to be followed if the Hematoma doesn’t subside immediately.
Immediate Management of Hematoma
Whenever local anesthesia is given, and this is followed by the formation of a swelling of any size, its advised to apply direct pressure on the site where there is the swelling or bleeding or the accumulation of blood. For most of the cases, the blood vessel lies in between the skin and bone, and when the injection leads to bleeding, the pressure has to be applied in these areas for more than 2 minutes. This way of management would effectively stops the bleeding.
Hematoma due to Inferior Alveolar Nerve Block: Whenever hematoma occurs due to the administration of the Inferior alveolar nerve block, the pressure has to be applied to the medial aspect of the mandibular ramus. Clinical manifestations of the hematoma are intraoral: possible tissue discoloration and probable tissue swelling on the medial (lingual) aspect of the mandibular ramus.
Hematoma due to Anterior Superior alveolar (Infraorbital) nerve block: Pressure has to be applied to the skin directly over the Infraorbital Foramen. Clinical manifestation is discoloration of the skin below the lower eye lid. Hematoma is unlikely to arise with Anterior Superior Alveolar nerve block because the technique described requires application of pressure to the injection site throughout drug administration and for a period of 2 to 3 minutes after, thus there is no potential injury or cause for Hematoma.
Hematoma due to Incisive (mental) nerve block: Just like the ASA nerve block, here the pressure is applied directly over the mental foramen, on the skin or mucous membrane while administering the local anesthesia, and thus the risk of Hematoma formation is largely reduced. Clinical manifestations are discoloration of skin over the mental foramen or swelling in the mucobuccal fold in the region of the mental foramen.
Hematoma due to Buccal nerve block or any palatal injection: Place pressure at the site of bleeding, and it would slowly get reduced. In these injections the clinical manifestations of hematoma are usually visible only within the mouth.
Hematoma due to Posterior superior alveolar nerve block: The Posterior Superior Alveolar (PSA) nerve block usually produces the largest and most esthetically unappealing Hematoma. The Infratemporal Fossa, into which bleeding occurs, is a place that can accommodate a large volume of blood. There is a colorless swelling that appears on the side of the face, usually a few minutes after the LA administration, and it is only then the Hematoma is recognized. The size increases over a period of days, both inferiorly and anteriorly towards the lower front region of the cheek. Due to the location of the blood vessels that are involved, it becomes difficult to apply pressure on the site where the bleeding is occurring. It is also relatively difficult to apply pressure directly to the posterior superior alveolar artery (the primary source of bleeding), the facial artery, and the pterygoid plexus of veins. They are located posterior, superior, and medial to the maxillary tuberosity. Bleeding normally ceases when external pressure on the vessels exceeds the internal pressure or when clotting occurs. Digital pressure can be applied to the soft tissues in the mucobuccal fold as far distally as can be tolerated by the patient (without eliciting a gag reflex). Apply pressure in a medial and superior direction. If available, ice should be applied (extraorally) to increase pressure on the site and help constrict the vessel.
Subsequent Management of Hematoma
- Once you have identified Hematoma, and the immediate steps are taken, the patient may be discharged after the bleeding stops. Note the hematoma on the patient’s dental chart.
Advise the patient about possible soreness and limitation of movement (trismus). If either of these develops, begin treatment as described for trismus. There will likely be discoloration as a result of extravascular blood elements, which gradually gets resorbed over 7 to 14 days. - If there is any soreness, advise the patient to have any analgesic such as Aspirin. After the incident, try to avoid applying heat to that area for at least 6 hours, because heat produces vasodilation, and this may further increase the size of the Hematoma. Heat may be applied to the region beginning the next day. It serves as an analgesic, and its vasodilating properties may increase the rate at which blood elements are resorbed, although its benefits are debatable.
- The patient should apply warm moist towels to the affected area for 20 minutes every hour.
- After the recognition of the hematoma formation, initially Ice may be applied, as it would act as both an analgesic and a vasoconstrictor, and it may aid in minimizing the size of the hematoma.
- Time (tincture of time) is the most important element in managing a hematoma. With or without treatment, a hematoma will be present for 7 to 14 days. Avoid additional dental therapy in the region until symptoms and signs resolve.
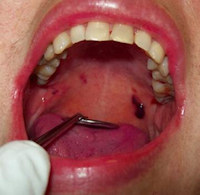
very nice . thanks to dr. chetan .
Thank you dr, i have a question, if hematoma after administration of local anesthesia, do we have to give antibiotic to prevent any infection? If yes, is it topical or systemic and how long the duration? Thank you
since Aspirin has anti-platelete activity how we can prescribe it in haematoma?
Could you pl. let me have the picture of hematoma to be used in a tect book I’m writing for dental students at my faculty.
Thanks so much for this info! I had dental work done yesterday, and my cheek was unusually swollen, and it was difficult to move my jaw. Today, my cheek is turning purple. Your article was the only good information I could find on what was happening to me, and what I should do about it. Much appreciated!